ADHD in Children: Why Your Child Needs to Understand Their Own Brain
We spend enormous energy helping parents understand ADHD, and adjusting school environments. But research shows the missing — and most powerful — intervention is helping the child understand themselves.
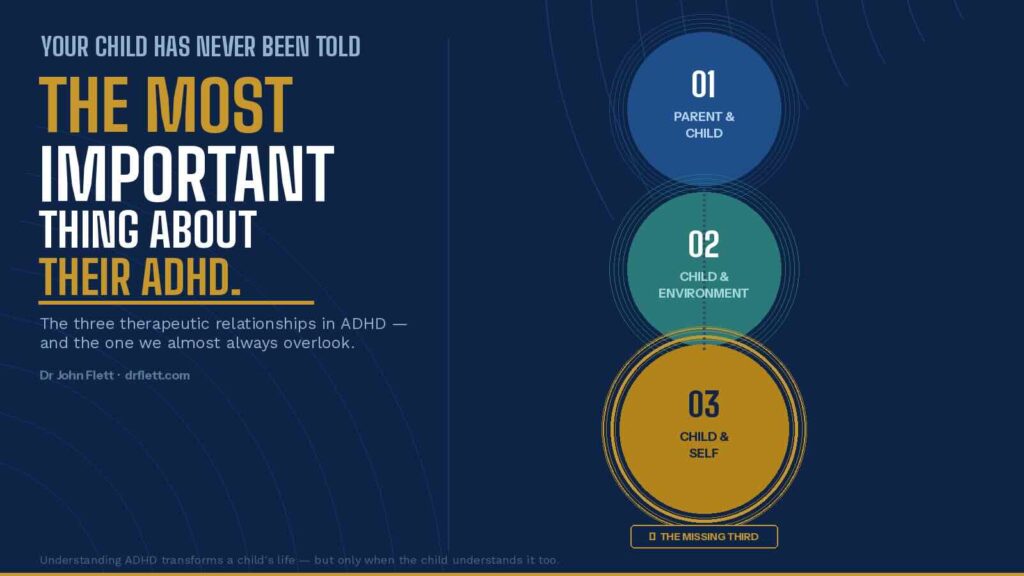
For decades, the management of ADHD has rested on two foundations: helping parents understand their child, and adjusting the environments in which that child operates. Both are essential. Both are evidence-based. But there is a third relationship that is almost entirely overlooked — and it may be the most important one of all. It is the relationship the child has with themselves.
A child who does not understand why they think, feel, and behave as they do will inevitably fill that vacuum with the most painful explanation available: that they are broken, lazy, stupid, or simply not enough. This is not self-pity. It is the entirely rational conclusion of a mind trying to make sense of its own experience without a map.
This is a problem we can fix. And the evidence for doing so is compelling.
The Three Therapeutic Relationships in ADHD Management
When a child with ADHD sits in a clinical consultation, the visible conversation is between clinician, child, and parent. But the treatment that truly transforms a life happens in three distinct relational spaces — and all three must be cultivated if we are to achieve the outcomes our patients deserve.
The Parent-Child Relationship: Shifting from “Won’t” to “Can’t”
The most transformative shift a parent can make is deceptively simple: moving from understanding their child’s ADHD difficulties as motivational to understanding them as neurological.
When a parent genuinely grasps that their child cannot yet reliably do the thing being asked of them, the emotional climate of the household changes. Not because expectations are lowered — but because the quality of the parental response changes entirely.
“Why won’t you just listen?” becomes “What does my child need to help their brain do this?” That single shift — from accusation to curiosity — is worth more than most therapeutic interventions combined.
Russell Barkley’s foundational work establishes that ADHD is not a disorder of knowing what to do — it is a disorder of doing what you know, when and where it matters most. The child who can tell you exactly how they should behave, and then immediately fails to, is not being manipulative. They are demonstrating the core executive function deficit in real time.
Ross Greene’s collaborative problem-solving model builds on the same insight: children do well when they can. When they can’t, the question isn’t “what’s wrong with this child?” — it’s “what skill is missing, and how do we build it?”
The parent who truly understands is the intervention that goes home with the child — present every hour of every day, including all the hours when no clinician or therapist is anywhere near.
The Child-Environment Relationship: Scaffolding the Brain Can’t Yet Provide
ADHD is, at its neurological core, a disorder of executive function — the brain’s capacity to plan, initiate, sustain, shift, and regulate. The prefrontal cortex that orchestrates these functions develops approximately three to four years later in children with ADHD than in their neurotypical peers.
The practical implication is profound: many of the demands we routinely place on children with ADHD are developmentally unrealistic. We are asking a ten-year-old brain to perform with the self-regulatory capacity of a seven-year-old — and then interpreting the predictable failure as a character problem.
External structure compensates for internal regulation deficits. Visual schedules, predictable routines, chunked tasks, movement breaks, and checklists are not concessions — they are prosthetics for executive function, doing externally what the prefrontal cortex cannot yet reliably do from within.
School accommodations are not privilege — they are equalisation. Extended time, preferential seating, and reduced working memory load do not give a child with ADHD an advantage. They remove a neurological disadvantage. Parents who understand this become confident advocates rather than apologetic supplicants.
The Child-Self Relationship: The Missing Third — and Why It Changes Everything
We have spent decades refining our ability to help parents understand their children. We have built entire fields of practice around modifying environments and implementing educational accommodations. These efforts have genuinely helped many children.
But we have paid almost no systematic attention to what may be the most important therapeutic target of all: helping the child understand themselves.
The Cancer Analogy: Why Unexplained Suffering Is Uniquely Harmful
Consider a person experiencing profound fatigue, weight loss, pain, and declining function — and nobody tells them why. Their mind does not sit quietly in that vacuum. It fills it with explanation. And for a suffering mind working without information, those explanations are rarely kind.
Now consider the child with ADHD who has no framework for their experience. They cannot sustain attention when others can. They cannot control their impulses when it seems obvious they should. They lose things, forget things, start things and abandon them, disrupt classrooms, disappoint parents, frustrate teachers.
Without an explanatory framework, the child’s mind fills the vacuum with the most available explanation: “I am lazy. I am stupid. I am broken. I am not enough.” This is not self-pity — it is the entirely rational conclusion of a mind trying to make sense of its experience with the only tools it has.
And without intervention, this conclusion hardens into identity — with consequences that medication cannot reverse and accommodations cannot undo.
The ADHD diagnosis, offered at the right level and in the right relational context, does something no other intervention can: it externalises what the child has been internalising. It separates the condition from the self. And that separation is not merely psychological comfort — it is the prerequisite for agency.
You cannot change what you believe is you.
You can only change what you understand affects you.
Why Clinicians Don’t Do This — and Why That Must Change
Fear of burdening the child with a label. Well-intentioned, but not supported by the evidence. Children who receive clear, age-appropriate explanations of their ADHD diagnosis consistently report relief, not distress. The burden was already there. The diagnosis names what they were already experiencing.
Not knowing how. Consultations are time-limited. The language is difficult to calibrate across ages. Very few clinicians have been trained in child-directed psychoeducation as a deliberate clinical skill. This is a training gap — not a reason for indefinite deferral.
Uncertainty about readiness. A legitimate clinical consideration that is too often used as a reason to delay indefinitely rather than to calibrate developmentally.
There is no age too young to begin receiving the truth about yourself — provided it is offered with warmth, accuracy, and hope. The question is never whether to tell a child. It is only how.
What the Research Shows: The Evidence for Child Self-Understanding in ADHD
The evidence base for child-directed ADHD psychoeducation, while still less extensive than parent-focused literature, is consistent and compelling.
Antshel & Barkley
Children who receive age-appropriate psychoeducation show improved treatment engagement, better medication adherence in adolescence, and — critically — reduced self-blame. Framework creates attribution shift.
Solanto — Metacognitive Therapy
Teaching young people how their executive function differs — not merely that it differs — produces self-regulation gains beyond what medication alone achieves. Understanding the mechanism drives strategy uptake.
Siegel — “Name It to Tame It”
When children can label and explain their internal experience, prefrontal cortex activity increases and amygdala response is modulated. Naming is neurologically regulatory, not just emotionally helpful.
Deci & Ryan — Self-Determination
Autonomous motivation — acting from genuine understanding of why something matters — produces qualitatively different and more durable outcomes than external, controlled motivation.
Tangney — Shame Research
Shame (“I am bad”) predicts resistance to change; guilt (“I did something bad”) predicts repair. Shame is the single greatest predictor of poor long-term ADHD outcomes — greater than symptom severity.
Hallowell & Ratey
The adolescent given language for their ADHD experience undergoes a qualitative shift in self-concept that medication alone cannot produce. Identity formation and self-understanding are inseparable in adolescence.
Understanding Your ADHD: A Guide for Young People at Every Age
The sections below are written directly for children and young people. They can be shared in a clinical consultation, read together with a parent, or given to a young person to explore on their own. The language is calibrated for each developmental stage — but the message throughout is the same.
You know what? Everybody’s brain is a little bit different — just like some people have curly hair and some have straight hair. Brains come in different shapes on the inside too.
Your brain is a very busy brain. It loves excitement and interesting things. And sometimes it’s very hard to sit still, wait your turn, or keep your feelings small when they want to be big.
That’s not because you are naughty. It’s not because you are bad. It’s just because of how your brain was made. And lots of kids have a brain that works exactly like yours.
There’s a name for it — it’s called ADHD. What it means is simple: your brain finds it harder to wait and concentrate on boring things — and much easier to concentrate on things you really love. Have you noticed how you can focus for ages on something you enjoy? That’s your brain too. It works in a special way.
“My brain is just being my brain. I can ask for help. And I am going to be okay.”
ADHD doesn’t mean you’re stupid, lazy, or bad. It means your brain is wired differently — like how different computers run different operating systems. They can all do great things, but they don’t work exactly the same way.
There’s a part of your brain called the prefrontal cortex — right behind your forehead. It’s like the conductor of an orchestra: it helps you plan, start things, keep going, and manage your feelings. In ADHD brains, this part develops a bit more slowly. So it’s not that you won’t do those things — it’s that your brain genuinely finds them harder. That’s a huge difference.
Think of it this way: you have a Ferrari engine — loads of power, speed, and energy. But the brakes are still being fitted. That’s ADHD. The engine is incredible. The brakes just need some extra work.
Here’s what most people forget to mention: the same brain that makes some things harder also does things other brains can’t do as easily. Hyperfocus, creativity, extraordinary energy, deep empathy, the courage to try things first — these are real ADHD strengths. Once you understand your brain, you can stop blaming yourself for things that aren’t your fault — and put your energy into the things that actually help.
Being told you have ADHD can feel complicated — a relief, a label you didn’t ask for, maybe both at once. Whatever you’re feeling is valid. But here’s what matters: understanding your ADHD — really understanding it, not just knowing the word — might be one of the most useful things you ever do for yourself.
ADHD is not a problem of knowing what to do. It’s a problem of doing what you know, in the moment it matters. You probably know you should start that assignment. The problem isn’t knowledge — it’s your brain’s ability to translate intention into action at the right time. When teachers say “you could do this if you tried harder,” they’re often simply wrong. Trying harder is not the solution to an executive function deficit — that’s like trying harder to see without glasses.
The biggest threat to long-term outcomes in ADHD is not the ADHD itself — it’s shame. Shame says “I am wrong, there’s nothing to fix.” Understanding your ADHD is the beginning of separating the condition from yourself. That separation is what makes real change possible.
Your job is not to overcome your ADHD. It is to understand it well enough to direct it. That is a fundamentally different — and infinitely more sustainable — relationship with your own brain.
At this stage of life, self-understanding is no longer a luxury — it’s an operational necessity. The external scaffolding of childhood is withdrawing. What replaces it has to come from within. For someone with ADHD, this transition is one of the most challenging and consequential they will face — and also, with the right understanding, one of the most transformative.
ADHD affects specific neurological systems — not your intelligence, character, or potential. It affects working memory, response inhibition, emotional regulation, task initiation, sustained attention, and time perception. It does not diminish your creativity, your capacity for connection, your courage, your humour, or your ability to be extraordinary at the things you love. Often, the same neurology enhances these.
A young adult who understands why a strategy works — and has chosen it as a tool that serves their own goals — will maintain it through difficulty. One who’s simply complying because someone told them to will abandon it at the first inconvenience. This is the difference self-understanding makes.
You have, in all likelihood, worked harder than most of the people around you — with less neurological support, less environmental accommodation, and less understanding of why things were difficult. That is not nothing. That is, in fact, a form of extraordinary resilience. And it deserves to be named as such.
Frequently Asked Questions About ADHD and Child Self-Understanding
What are the three therapeutic relationships in ADHD management?
The three therapeutic relationships in ADHD management are: (1) the Parent-Child relationship — how the parent understands and responds to their child’s ADHD; (2) the Child-Environment relationship — how school, structure, and routines are adjusted to support the child’s neurology; and (3) the Child-Self relationship — how the child themselves understands their own ADHD, identity, and neurological profile. The third is the most neglected in clinical practice, and may be the most important for long-term outcomes.
Why is it important for children with ADHD to understand their own diagnosis?
Children who don’t understand their ADHD tend to attribute their difficulties to personal failure — concluding that they are lazy, stupid, or broken. Research by Antshel and Barkley shows that age-appropriate psychoeducation reduces self-blame, improves treatment engagement, and leads to better long-term outcomes. Daniel Siegel’s work demonstrates that naming and explaining an experience is neurologically regulatory — it activates the prefrontal cortex and helps children manage their responses more effectively.
How does shame affect children with ADHD?
Research by June Price Tangney shows that shame — the belief that “I am bad” rather than “I did something bad” — is the single greatest predictor of poor long-term outcomes in ADHD, outranking even symptom severity. Shame makes children resistant to the very strategies that could help them, because trying to change implies confirming what they already secretly believe. An age-appropriate explanation of the ADHD diagnosis is the most powerful antidote, because it recontextualises years of difficulty as neurological rather than characterological.
At what age should a child with ADHD be told about their diagnosis?
There is no age too young to begin receiving an honest, age-appropriate explanation of their ADHD. The question is never whether to tell a child, but how — using language and concepts calibrated to their developmental stage. Children as young as five or six can understand that their brain works differently in ways that explain — without excusing — their challenges. The evidence consistently shows that children who receive clear explanations report relief, not distress.
What does “ADHD is a can’t, not a won’t” mean?
This phrase, drawn from Russell Barkley’s foundational research, captures a critical distinction: ADHD is not a disorder of knowing what to do — it is a disorder of doing what you know, in the moment it matters. The child who can explain exactly how they should behave, and then immediately fails to, is not being defiant. They are demonstrating a core executive function deficit. Shifting from “won’t” (motivational) to “can’t” (neurological) changes the parental response from frustration to problem-solving — and the child’s experience from shame to understanding.
Does Dr John Flett see ADHD patients in KwaZulu-Natal?
Yes. Dr John Flett is a specialist paediatrician practising at The Assessment Centre in Kloof, KwaZulu-Natal, South Africa. He specialises in comprehensive ADHD assessments and neurodevelopmental medicine for children, adolescents, and young adults up to age 25 and beyond. He also provides family guidance, school accommodation letters, and parent education. For appointments and referrals, visit drflett.com.
The Most Important Beginning
The parent who understands their child is transformative. The environment engineered to support that child is essential. But the child who understands themselves — who has language for their experience, who can separate their condition from their character, who knows what their brain needs and how to ask for it — that child carries something into adulthood that no prescription, no accommodation, and no amount of external scaffolding can provide.
Understanding changes everything. Not just for parents. For the child.
There is no age too young to begin receiving the truth about yourself — provided it is offered with warmth, accuracy, and hope. That offering is one of the most important things a clinician or a parent can ever give.
Book an ADHD Assessment in Kloof, KwaZulu-Natal
Dr John Flett offers comprehensive ADHD assessments for children, adolescents, and young adults at The Assessment Centre in Kloof. Assessments include age-appropriate psychoeducation, parent guidance, and school accommodation support.
Get in TouchDr Flett has over 25 years of clinical experience in ADHD and neurodevelopmental medicine, practising at The Assessment Centre in Kloof, KwaZulu-Natal. His core clinical philosophy: parental — and personal — understanding is the most powerful therapeutic intervention. drflett.com · guidelittleminds.com